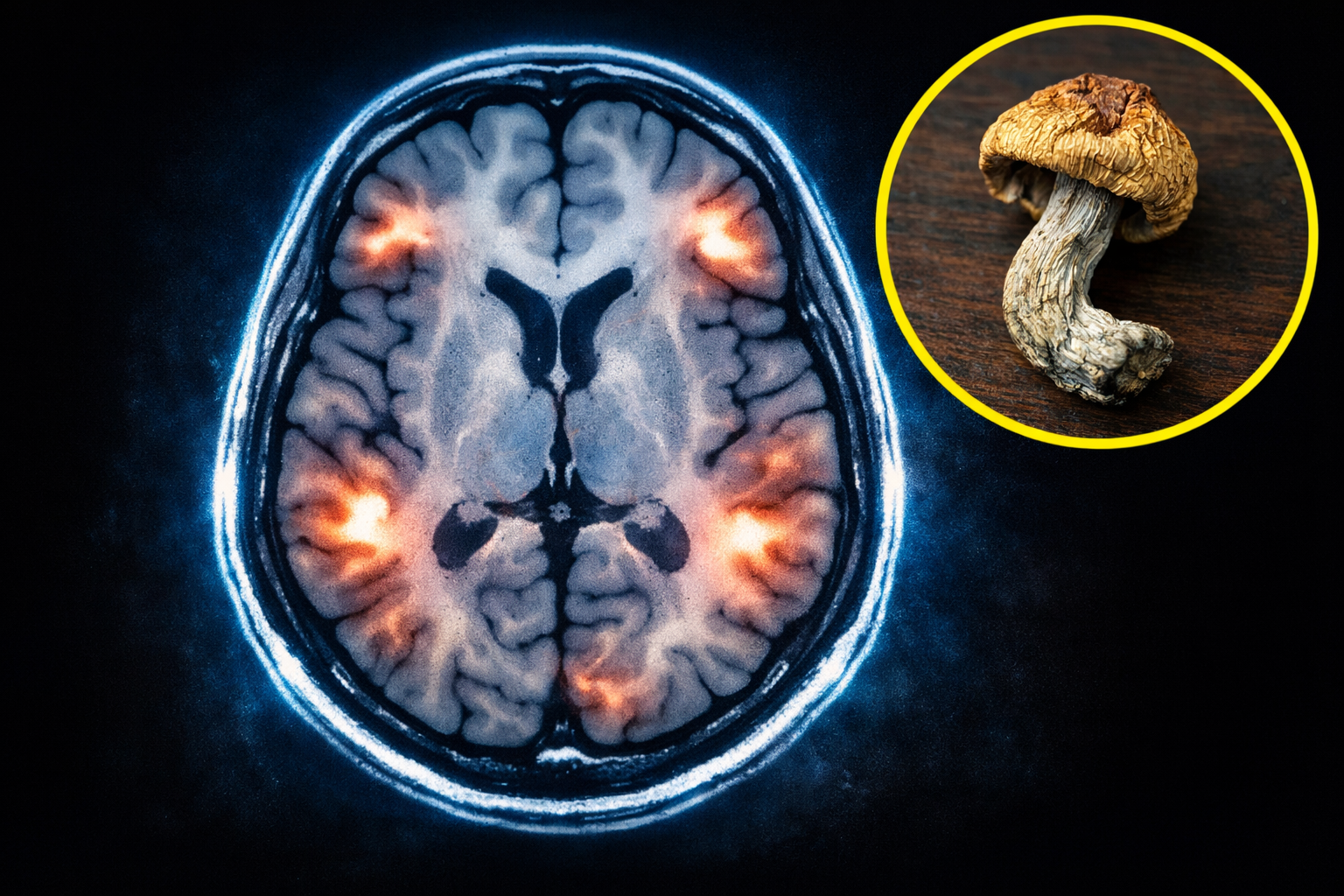
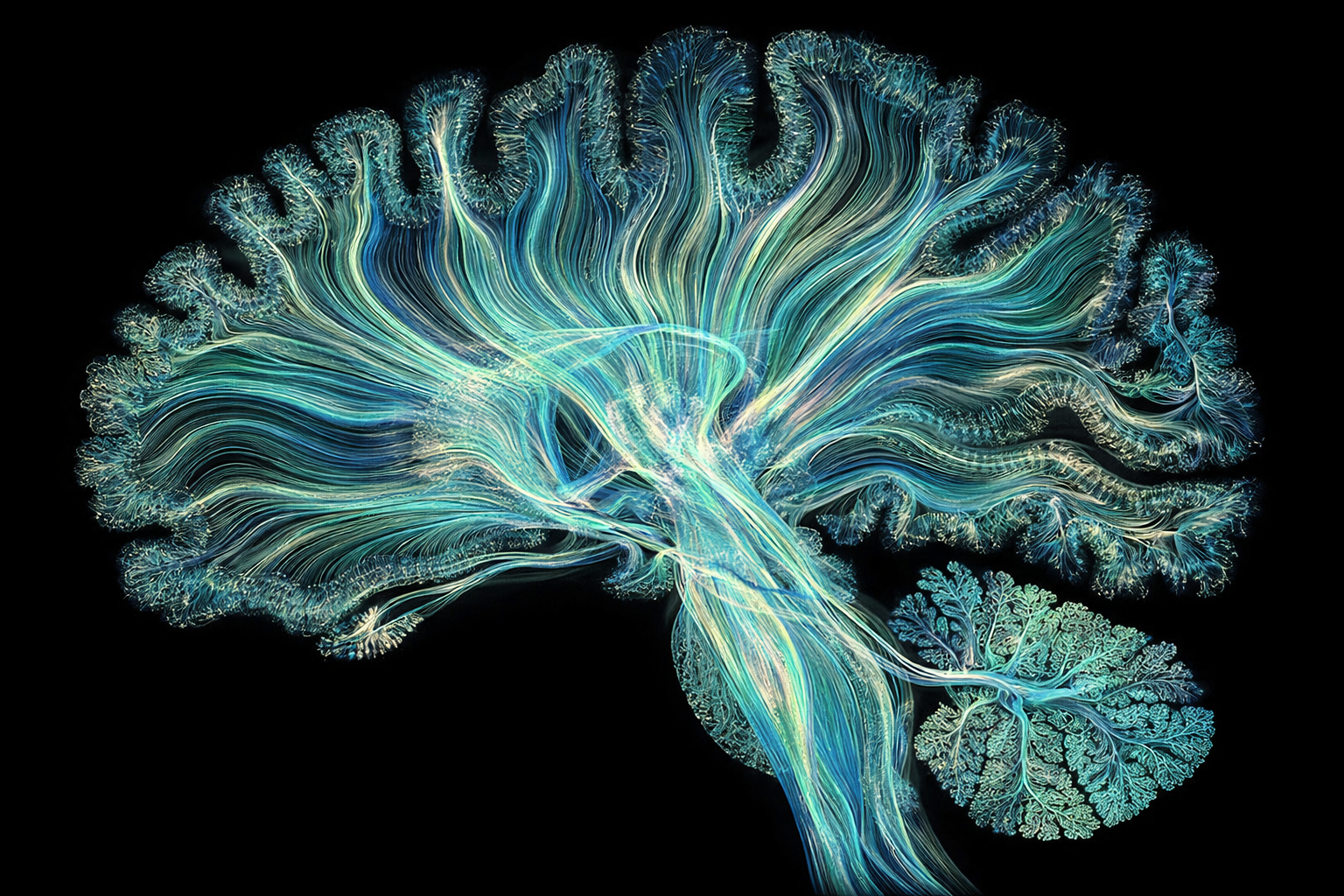
A healthy brain is an adaptive network. It responds to new information, updates its patterns, and finds more efficient ways to organise itself over time. Mental illness, in many cases, looks like the opposite of that: a network that has lost its flexibility, committed its resources to a fixed pattern of activation, and can no longer revise itself in response to a changing environment.
OCD is one of the clearest examples of this kind of pathological rigidity, and a new clinical trial suggests psilocybin may be able to restore some of what has been lost.
Published in the Journal of Psychopharmacology in March 2026, a randomised trial from the University of Arizona gave fifteen people with treatment-refractory OCD up to eight weekly high-dose psilocybin sessions over two months. At the end of the protocol, 73% met the clinical threshold for response (at least a 35% reduction in Yale-Brown Obsessive Compulsive Scale scores), and 40% reached full remission. Those gains held at six months, with no serious adverse events.
There are caveats. There were only participants and the blinding was almost certainly compromised because high-dose psilocybin is difficult to mistake for a lorazepam placebo. This is preliminary evidence. What it does offer is a strong enough signal to take the underlying mechanism seriously, and the mechanism is where the interesting questions live.
The Vicious Circle Of OCD
OCD can be understood as a brain that has organised itself around threat. The orbitofrontal cortex generates an error signal, the thalamus amplifies it, the striatum drives a compulsive response, and the whole sequence loops back on itself without resolution. Neuroimaging studies show measurably elevated metabolic activity in this network in people with OCD. And what makes the condition so resistant to treatment is that the pattern is self-reinforcing. Every repetition of the loop deepens it. The network has, in effect, learned to be stuck.
SSRIs adjust the serotonin environment broadly, and they help roughly 40-60% of patients see meaningful improvement. But the mechanism is indirect. It doesn’t restore the network’s capacity to reorganise. For people who’ve already failed multiple interventions, as all participants in the recent trial had, the response rates are considerably worse. The tool doesn’t match the problem.
Earlier psilocybin research had already shown that even a moderate 10mg dose produced clinically significant reductions in compulsive behaviour, but rigorous evidence for repeated dosing in a treatment-refractory population was still missing.
If you’re interested in the evolving story of fungi, psychedelics, and nature’s intelligence, our weekly newsletter The Spore Report is worth your time.
Read The Spore Report →Disruption as Medicine
Psilocybin works differently, and the difference is worth understanding at the level of what it actually does to a living network.
Psilocybin’s active metabolite, psilocin, binds to serotonin 5-HT2A receptors concentrated in the prefrontal cortex, orbitofrontal cortex, and thalamus. This disrupts thalamic gating, the process by which the thalamus filters what information reaches the cortex and at what intensity.
In OCD, that filter is locked, relaying the same error signal on repeat. Psilocybin temporarily overrides it, flooding the cortex with input from pathways that are normally suppressed and producing a sharp increase in neural entropy. The brain’s habitual connectivity patterns loosen. The default mode network, closely tied to the maintenance of fixed self-referential patterns, drops in activity. The network’s normal signal hierarchy, including the rigid loop that characterises OCD, is temporarily dissolved.
This is closer to a controlled burn than a medication. Rather than adjusting the chemistry around a stuck pattern, psilocybin interrupts the pattern’s structural basis directly, creating a window in which the network can reorganise.
There is also growing evidence that psilocybin drives increases in BDNF (brain-derived neurotrophic factor), the signalling molecule most associated with synaptic growth and structural plasticity, and that dendritic spine remodelling occurs in the medial prefrontal cortex following administration. So the network is not only loosening. It’s also physically rebuilding itself.
Why Eight Sessions?
The trial’s repeated-dose design is significant here, and it’s arguably the most interesting feature of the study. A Yale single-dose RCT showed durable symptom reductions from one session alone, which raises the question of what eight sessions might do differently. Classic psychedelics produce acute tolerance within 24-48 hours, so the therapeutic effect almost certainly isn’t the acute experience accumulating in a straightforward way. Something else is building across the eight weeks.
One plausible reading is that each session extends the neuroplasticity window a little further, allowing structural changes to accumulate before the old pattern can fully reassert itself. A single disruption opens a gap, but repeated disruptions, spaced weekly, may hold that gap open long enough for deeper reorganisation to take root.
What grows back during that window is a question the trial doesn’t answer. The participants received non-directive support rather than formal psychotherapy, which raises the possibility that pairing repeated dosing with more deliberate integration work could improve on these results further.
What This Suggests
The mechanism outlined here is coherent but partly inferential. The trial didn’t include neuroimaging, so we can’t confirm that network activity actually normalised in the people who responded, and the small sample means the findings need replication in larger trials before drawing firm conclusions.
What the results do suggest is that the brain’s capacity for adaptive reorganisation, even after decades of pathological rigidity, may be more recoverable than the limits of current pharmacology imply.
Psilocybin seems to work not by correcting a chemical deficiency but by temporarily restoring the conditions under which a living network can revise itself. For a condition defined by the loss of that capacity, that framing may matter as much as the mechanism.
If this framing resonates, the ideas here sit at the heart of The Decentralised Brain Protocol, a guide to understanding your brain as a living network rather than a machine, and what that means for how you think about health, habit, and change.
If you’re interested in the evolving story of fungi, psychedelics, and nature’s intelligence, our weekly newsletter The Spore Report is worth your time.
Read The Spore Report →